It can often be harmless and pain-free, but at times it can bring discomfort and pain.
In this article, we investigate what a hernia is, the common causes of hernia, and how they are treated.
Here are some key points about hernias. More detail and supporting information is in the main article.
- Hernias often produce no troublesome symptoms, but abdominal complaints may signal a serious problem.
- They are usually straightforward to diagnose, simply by feeling and looking for the bulge.
- Treatment is a choice between watchful waiting and corrective surgery, either via an open or keyhole operation.
- Inguinal hernia surgery is more common in childhood and old age, while the likelihood of femoral hernia surgery increases throughout life.
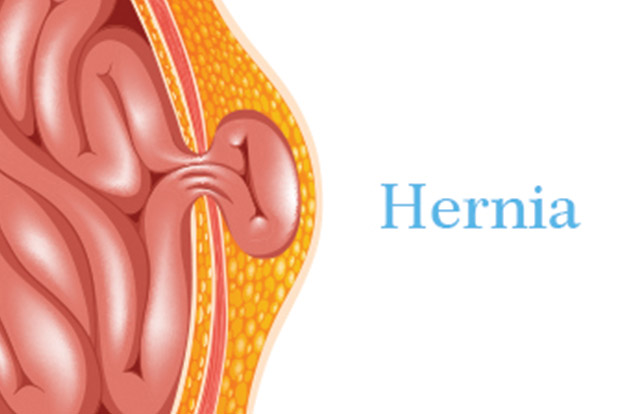
What is a hernia?
A hernia occurs when there is a weakness or hole in the peritoneum, the muscular wall that usually keeps abdominal organs in place.
This defect in the peritoneum allows organs and tissues to push through, or herniate, producing a bulge.
The lump may disappear when the person lies down, and sometimes it can be pushed back into. Coughing may make it reappear.

how to Treat Hernia /Piles / Knee Replacement / Urology stone in Sanket Surgical Hospital
Hernias can commonly be found in the following areas:
Groin: a femoral hernia creates a bulge just below the groin. This is more common in women. An inguinal hernia is more common in men. It is a bulge in the groin that may reach the scrotum.
Upper part of the stomach: a hiatal or hiatus hernia is caused by the upper part of the stomach pushing out of the abdominal cavity and into the chest cavity through an opening in the diaphragm.
Belly button: a bulge in this region is produced by an umbilical or periumbilical hernia.
Surgical scar: past abdominal surgery can lead to an incisional hernia through the scar.
Causes
With the exception of an incisional hernia (a complication of abdominal surgery), in most cases, there is no obvious reason for a hernia to occur. The risk of hernia increases with age and occurs more commonly in men than in women.
A hernia can be congenital (present at birth) or develop in children who have a weakness in their abdominal wall.
Activities and medical problems that increase pressure on the abdominal wall can lead to a hernia. These include:
- straining on the toilet (due to long-term constipation, for example)
- persistent cough
- cystic fibrosis
- enlarged prostate
- straining to urinate
- being overweight or obese
- abdominal fluid
- lifting heavy items
- peritoneal dialysis
- poor nutrition
- smoking
- physical exertion
- undescended testicles
Risk factors for hernia
The risk factors can be broken down by hernia type:
Incisional hernia risk factors
Because an incisional hernia is the result of surgery, the clearest risk factor is a recent surgical procedure on the abdomen.
People are most susceptible 3-6 months after the procedure, especially if:
- they are involved in strenuous activity
- have gained additional weight
- become pregnant
These factors all put extra stress on tissue as it heals.
Inguinal hernia risk factors
Those with a higher risk of inguinal hernia incude Smoking tobacco increases the risk of inguinal hernias.
- older adults
- people with close relatives who have had inguinal hernias
- people who have had inguinal hernias previously
- males
- smokers, as chemicals in tobacco weaken tissues, making a hernia more likely
- people with chronic constipation
- premature birth and low birth weight
- pregnancy
Umbilical hernia risk factors
Umbilical hernias are most common in babies with a low birth weight and premature babies.
In adults, the risk factors include:
- being overweight
- having multiple pregnancies
- being female
Hiatal hernia risk factors
The risk of hiatal hernia is higher in people who:
- are aged 50 years or over
- have obesity
In many cases, a hernia is no more than a painless swelling that presents no problems and needs no immediate medical attention.
how to Treat Hernia /Piles / Knee Replacement / Urology stone in Sanket Surgical Hospital
A hernia may, however, be the cause of discomfort and pain, with symptoms often becoming worse when standing, straining, or lifting heavy items. Most people who notice increasing swelling or soreness eventually see a doctor.
In some cases, a hernia needs immediate surgery, for instance, when part of the gut becomes obstructed or strangulated by an inguinal hernia.
Immediate medical attention should be sought if an inguinal hernia produces acute abdominal complaints such as:
- pain
- nausea
- vomiting
- the bulge cannot be pushed back into the abdomen
The swelling, in these cases, is typically firm and tender and cannot be pushed back up into the abdomen.
A hiatal hernia can produce symptoms of acid reflux, such as heartburn, which is caused by stomach acid getting into the esophagus.
Treatment
For a hernia without symptoms, the usual course of action is to watch and wait, but this can be risky for certain types of hernia, such as femoral hernias.
Within 2 years of a femoral hernia being diagnosed, 40 percent result in bowel strangulation.
It remains unclear whether non-emergency surgery is worthwhile for hernia repair in cases of an inguinal hernia without symptoms that can be pushed back into the abdomen.
The American College of Surgeons and some other medical bodies consider elective surgery unnecessary in such cases, recommending instead a course of watchful waiting.
Others recommend surgical repair to remove the risk of later strangulation of the gut, a complication where blood supply is cut off to an area of tissue, which requires an emergency procedure.
These health authorities consider an earlier, routine operation preferable to a more risky emergency procedure.
how to Treat Hernia /Piles / Knee Replacement / Urology stone in Sanket Surgical Hospital
Types of surgery
Although surgical options depend on individual circumstances, including the location of the hernia, there are two main types of surgical intervention for hernia:
- open surgery
- laparoscopic operation (keyhole surgery)
Open surgical repair closes the hernia using sutures, mesh, or both, and the surgical wound in the skin is closed with sutures, staples, or surgical glue.
Laparoscopic repair is used for repeat operations to avoid previous scars, and while usually more expensive, is less likely to cause complications such as infection.
Surgical repair of a hernia guided by a laparoscope allows for the use of smaller incisions, enabling a faster recovery from the operation.
The hernia is repaired in the same way as in open surgery, but it is guided by a small camera and a light introduced through a tube. Surgical instruments are inserted through another small incision. The abdomen is inflated with gas to help the surgeon see better and give them space to work; the whole operation is performed under general anesthetic.
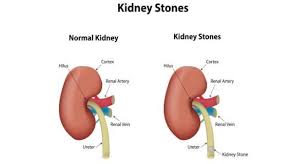
Kidney stones are the result of a buildup of dissolved minerals on the inner lining of the kidneys.
They usually consist of calcium oxalate but may be composed of several other compounds.
Kidney stones can grow to the size of a golf ball while maintaining a sharp, crystalline structure.
The stones may be small and pass unnoticed through the urinary tract, but they can also cause extreme pain as they leave the body.
how to Treat Hernia /Piles / Knee Replacement / Urology stone in Sanket Surgical Hospital
Symptoms
A kidney stone usually remains symptomless until it moves into the ureter. When symptoms of kidney stones become apparent, they commonly include:
- severe pain in the groin and/or side
- blood in urine
- vomiting and nausea
- white blood cells or pus in the urine
- reduced amount of urine excreted
- burning sensation during urination
- persistent urge to urinate
- fever and chills if there is an infection
Complications
Kidney stones that remain inside the body can also lead to many complications, including blockage of the the tube connecting the kidney to the bladder, which obstructs the path that urine uses to leave the body.
According to research, people with kidney stones have a significantly higher risk of developing chronic kidney disease.
Causes
The leading cause of kidney stones is a lack of water in the body.
Stones are more commonly found in individuals who drink less than the recommended eight to ten glasses of water a day.
When there is not enough water to dilute the uric acid, a component of urine, the urine becomes more acidic.
An excessively acidic environment in urine can lead to the formation of kidney stones.
Medical conditions such as Crohn’s disease, urinary tract infections, renal tubular acidosis, hyperparathyroidism, medullary sponge kidney, and Dent’s disease increase the risk of kidney stones.
Risk factors
Kidney stones are more common among males than females. Most people who experience kidney stones do so between the ages of 30 and 50 years. A family history of kidney stones also increases one’s chances of developing them.
Similarly, a previous kidney stone occurrence increases the risk that a person will develop subsequent stones in the future if preventative action is not taken.
Certain medications can increase the risk of developing kidney stones. Scientists found that topiramate (Topamax), a drug commonly prescribed to treat seizures and migraine headaches, can increase the likelihood of kidney stones developing.
Additionally, it is possible that long-term use of vitamin D and calcium supplements cause high calcium levels, which can contribute to kidney stones.
Additional risk factors for kidney stones include diets that are high in protein and sodium but low in calcium, a sedentary lifestyle, obesity, high blood pressure, and conditions that affect how calcium is absorbed in the body such as gastric bypass surgery, inflammatory bowel disease, and chronic diarrhea.
Treatment
Treating kidney stones is primarily focused on symptom management. Passing a stone can be very painful.
If a person has a history of kidney stones, home treatment may be suitable. Individuals who have never passed a kidney stone should speak with a doctor.
If hospital treatment is needed, an individual may be rehydrated via an intravenous (IV) tube, and anti-inflammatory medication may also be administered.
Narcotics are often used in an effort to make the pain of passing the stone tolerable. Antiemetic medication can be used in people experiencing nausea and vomiting.
In some cases, a urologist can perform a shock wave therapy called lithotripsy. This is a treatment that breaks the kidney stone into smaller pieces and allow it to pass.
People with large stones located in regions that do not allow for lithotripsy may receive surgical procedures, such as removal of the stone via an incision in the back or by inserting a thin tube into the urethra.
Home remedies
There are a few steps that can be taken to reduce the impact of kidney stones and assist doctors in providing treatment.
The first is drinking enough water to make the urine completely clear. A person can tell they are not consuming enough water if their urine is yellow or brown.
A doctor may also request that a kidney stone is passed naturally though urinating. They will then ask that you retrieved a kidney stone from the urine by filtering it through a stocking or gauze.
On studying the retrieved stone, they will be able to determine what further treatment is required.
Diet
There are several foods that have a positive impact on kidney health. These can help reduce both the risk and impact of kidney stones. The body naturally passes the stone within 48 to 72 hours.
Kidney beans are one such option. Boil the pods inside the beans for around six hours, strain the liquid, and allow this liquid to cool.
People with kidney stones should consume this liquid every 2 hours over the course of 1 to 2 days.
Other foods that can protect the kidneys include:
- basil
- celery
- apples
- grapes
- pomegranates
Vitamin B6 supplements and pyroxidine supplements have also been recommended as effective treatments.
SymptomsIn most cases, the symptoms of piles are not serious. They normally resolve on their own after a few days.
An individual with piles may experience the following symptoms:
- A hard, possibly painful lump may be felt around the anus. It may contain coagulated blood. Piles that contain blood are called thrombosed external hemorrhoids.
- After passing a stool, a person with piles may experience the feeling that the bowels are still full.
- Bright red blood is visible after a bowel movement.
- The area around the anus is itchy, red, and sore.
- Pain occurs during the passing of a stool.
Piles can escalate into a more severe condition. This can include:
- excessive anal bleeding, also possibly leading to anemia
- infection
- fecal incontinence, or an inability to control bowel movements
- anal fistula, in which a new channel is created between the surface of the skin near the anus and the inside of the anus
- a strangulated hemorrhoid, in which the blood supply to the hemorrhoid is cut off, causing complications including infection or a blood clot
Piles is classified into four grades:
- Grade I: There are small inflammations, usually inside the lining of the anus. They are not visible.
- Grade II: Grade II piles are larger than grade I piles, but also remain inside the anus. They may get pushed out during the passing of stool, but they will return unaided.
- Grade III: These are also known as prolapsed hemorrhoids, and appear outside the anus. The individual may feel them hanging from the rectum, but they can be easily re-inserted.
- Grade IV: These cannot be pushed back in and need treatment. They are large and remain outside of the anus.
External piles form small lumps on the outside edge of the anus. They are very itchy and can become painful if a blood clot develops, as the blood clot can block the flow of blood. Thrombosed external piles, or hemorrhoids that have clotted, require immediate medical treatment.
Causes
Pregnancy may increase the risk of developing piles, as it causes increased pressure in the body.
Piles are caused by increased pressure in the lower rectum.
The blood vessels around the anus and in the rectum will stretch under pressure and may swell or bulge, forming piles. This may be due to:
- chronic constipation
- chronic diarrhea
- lifting heavy weights
- pregnancy
- straining when passing a stool
The tendency to develop piless may also be inherited and increases with age.
Diagnosis
A doctor can usually diagnose piles after carrying out a physical examination. They will examine the anus of the person with suspected piles.
The doctor may ask the following questions:
- Do any close relatives have piles?
- Has there been any blood or mucus in the stools?
- Has there been any recent weight loss?
- Have bowel movements changed recently?
- What color are the stools?
For internal piles, the doctor may perform a digital rectal examination (DRE) or use a proctoscope. A proctoscope is a hollow tube fitted with a light. It allows the doctor to see the anal canal up close. They can take a small tissue sample from inside the rectum. This can then be sent to the lab for analysis.
The physician may recommend a colonoscopy if the person with piles presents signs and symptoms that suggest another digestive system diseases, or they are demonstrating any risk factors for colorectal cancer.
Treatments
In the majority of cases, piles resolve on their own without the need for any treatment. However, some treatments can help significantly reduce the discomfort and itching that many people experience with piles.
Lifestyle changes
Diet and body weight may affect the risk of developing piles. Eating a high fiber diet and managing weight may help to prevent and treat the condition.
A doctor will initially recommend some lifestyle changes to manage piles.
Diet: Piles can occur due to straining during bowel movements. Excessive straining is the result of constipation. A change in diet can help keep the stools regular and soft. This involves eating more fiber, such as fruit and vegetables, or primarily eating bran-based breakfast cereals.
A doctor may also advise the person with piles to increase their water consumption. It is best to avoid caffeine.
Body weight: Losing weight may help reduce the incidence and severity of piles.
To prevent piles, doctors also advise exercising and avoiding straining to pass stools. Exercising is one of the main therapies for piles.
Medications

Several medicinal options are available to make symptoms more manageable for an individual with piles.
Over-the-counter (OTC) medications: These are available over-the counter or online. Medications include painkillers, ointments, creams, and pads, and can help soothe redness and swelling around the anus.
OTC remedies do not cure piles but can help the symptoms. Do not use them for more than 7 days in a row, as they can cause further irritation of the area and thinning of the skin. Do not use two or more medications at the same time unless advised to by a medical professional.
Corticosteroids: These can reduce inflammation and pain.
Laxatives: The doctor may prescribe laxatives if a person with piles suffers from constipation. These can help the person pass stools more easily and reduce pressure on the lower colon.
Surgical options
Around 1 in 10 people with piles will end up needing surgery.
Banding: The doctor places an elastic band around the base of the pile, cutting off its blood supply. After a few days, the hemorrhoid falls off. This is effective for treating all hemorrhoids of less than grade IV status.
Sclerotherapy: Medicine is injected to make the hemorrhoid shrink. The hemorrhoid eventually shrivels up. This is effective for grade II and III hemorrhoids and is an alternative to banding.
Infrared coagulation: Also referred to as infrared light coagulation, a device is used to burn the hemorrhoid tissue. This technique is used to treat grade I and II hemorrhoids.
Hemorrhoidectomy: The excess tissue that is causing the bleeding is surgically removed. This can be done in various ways and may involve a combination of a local anesthetic and sedation, a spinal anesthetic, or a general anesthetic. This type of surgery is the most effective for completely removing piles, but there is a risk of complications, including difficulties with passing stools, as well as urinary tract infections.
Hemorrhoid stapling: Blood flow is blocked to the hemorrhoid tissue. This procedure is usually less painful than hemorrhoidectomy. However, this procedure can lead to an increased risk of hemorrhoid recurrence and rectal prolapse, in which part of the rectum pushes out of the anus.